General Wellbeing, Health, Light
Light therapy and hypothyroidism
Thyroid issues are pervasive in modern society, affecting all genders and ages to varying degrees. Diagnoses are perhaps missed more often than any other condition and typical treatment/prescriptions for thyroid issues are decades behind the scientific understanding of the condition.
The question we are going to answer in this article is – Can light therapy play a role in prevention and treatment of thyroid/low metabolism problems?
Looking through scientific literature we see that light therapy’s effect on thyroid function has been studied dozens of times, in humans (e.g. Höfling DB et al., 2013), mice (e.g. Azevedo LH et al., 2005), rabbits (e.g. Weber JB et al., 2014), among others. To understand why light therapy may, or may not, be of interest to these researchers, first we need to understand the basics.
Contents
Introduction
Light therapy research on low thyroid people
Symptoms of low metabolic rate
Thyroid system basics
Bottom Line
Recommended Products
References
Medical & Healthcare Disclaimer
The information contained in this article is not intended or implicitly suggested to be an alternative for professional diagnoses, or profesionally recommended treatments & medical advice. Absolutely all of the content, including the article text itself, images, comments and other information, contained on this web page is for non-specific information purposes only. We strongly suggest that one should never ignore professional health/medical advice and we strongly suggest that one must not delay seeking a professionally recommended medical treatment because of information attained via reading this article/website. The products sold or recommended on this web site are absolutely not for the diagnosis, prevention, monitoring, treatment or alleviation of any specific disease, injury or disability.
Introduction
Hypothyroidism (low thyroid, underactive thyroid) should be considered more of a spectrum that everybody falls onto, rather than a black or white condition that only older people suffer from. Barely anyone in modern society has truely ideal thyroid hormone levels (Klaus Kapelari et al., 2007. Hershman JM et al., 1993. J. M. Corcoran et al., 1977.). Adding to the confusion, there are overlapping causes and symptoms with several other metabolic issues like diabetes, heart disease, IBS, high cholesterol, depression and even hair loss (Betsy, 2013. Kim EY, 2015. Islam S, 2008, Dorchy H, 1985.).
Having a ‘slow metabolism’ is in essence the same thing as hypothyroidism, which is why it coincides with other problems in the body. It’s only diagnosed as clinical hypothyroidism once it reaches a low point.
In a nutshell, hypothyroidism is the state of low energy production in the entire body as a result of low thyroid hormone activity. The typical causes are complex, including various diet and lifestyle factors such as; stress, heredity, ageing, polyunsaturated fats, low carbohydrate intake, low calorie intake, sleep deprivation, alcoholism, and even excess endurance exercise. Other factors such as thyroid removal surgery, fluoride intake, various medical therapies, and so on also cause hypothyroidism.
Light therapy potentially of aid to low thyroid people?
Red & infrared light (600-1000nm) may potentially be of use to metabolism in the body on several different levels.

- Some studies conclude that applying red light appropriately may improve production of the hormones. (Höfling et al., 2010,2012,2013. Azevedo LH et al., 2005. Вера Александровна, 2010. Gopkalova, I. 2010.) Like any tissue in the body, the thyroid gland requires energy to perform all of its functions. As thyroid hormone is a key component in stimulating energy production, you can see how a lack of it in the gland’s cells decreases further thyroid hormone production – a classic vicious cycle. Low thyroid -> low energy -> low thyroid -> etc.
- Light therapy when applied appropriately on the neck may potentially break this vicious cycle, in theory by improving local energy availability, thus increasing natural thyroid hormone production by the gland again. With a healthy thyroid gland restored, a host of positive downstream effects occur, as the entire body finally gets the energy it needs (Mendis-Handagama SM, 2005. Rajender S, 2011). Steroid hormone (testosterone, progesterone, etc.) synthesis picks up again – mood, libido and vitality are enhanced, body temperature increases and basically all symptoms of a low metabolism are reversed (Amy Warner et al., 2013) – even physical appearance and sexual attractiveness increases.
- Alongside potential systemic benefits from thyroid exposure, applying light anywhere on the body may also give systemic effects, via the blood (Ihsan FR, 2005. Rodrigo SM et al., 2009. Leal Junior EC et al., 2010). Although red blood cells have no mitochondria; blood platelets, white blood cells and other types of cells present in the blood do contain mitochondria. This alone is being studied to see how and why it may lower inflammation and cortisol levels – a stress hormone that prevents T4 -> T3 activation (Albertini et al., 2007).
- If one were to apply red light to specific areas of the body (such as the brain, skin, testes, wounds, etc.), some researchers hypothesise that it could perhaps give a more intense local boost. This is best shown by studies of light therapy on skin disorders, wounds and infections, where in various studies the healing time is potentially reduced by red or infrared light (J. Ty Hopkins et al., 2004. Avci et al., 2013, Mao HS, 2012. Percival SL, 2015. da Silva JP, 2010. Gupta A, 2014. Güngörmüş M, 2009). The local effect of light would seem to potentially be different yet complementary to the natural function of thyroid hormone.
The mainstream and generally accepted theory of light therapy’s direct impact involves cellular energy production. The effects are supposedly exerted primarily by photodissociating nitric oxide (NO) from the mitochondrial enzymes (cytochrome c oxidase, etc.). You can think of NO as a harmful competitor to oxygen, much like carbon monoxide is. NO basically shuts down energy production in cells, forming an extremely wasteful environment energetically, which downstream raises cortisol/stress. Red light is theorised to prevent this nitric oxide poisoning, and resulting stress, by removing it from mitochondria. In this way red light can be thought of as ‘protective negation of stress’, rather than immediately increasing energy production. It’s simply allowing your cells’ mitochondria to work properly by alleviating the dampening effects of stress, in a way that thyroid hormone alone doesn’t necessarily do.
So while thyroid hormone improves mitochondria counts and effectiveness, the hypothesis around light therapy is that it may enhance and ensure the effects of the thyroid by inhibiting the negative stress-related molecules. There may be several other indirect mechanisms by which both thyroid and red light reduce stress, but we won’t go into them here.
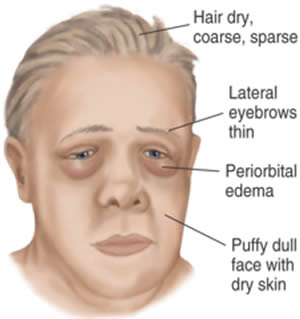
Symptoms of low metabolic rate/hypothyroidism
- Low heart rate (below 75 bpm)
- Low body temperature, less than 98°F/36.7°C
- Always feel cold (esp. hands and feet)
- Dry skin anywhere on body
- Moody / angry thoughts
- Feeling of stress / anxiety
- Brain fog, headaches
- Slow growing hair/fingernails
- Bowel issues (constipation, crohns, IBS, SIBO, bloating, heartburn, etc.)
- Frequent urination
- Low/no libido (and/or weak erections / poor vaginal lubrication)
- Yeast/candida susceptibility
- Inconsistent menstrual cycle, heavy, painful
- Infertility
- Rapidly thinning/receding hair. Thinning eyebrows
- Bad sleep
How does the thyroid system work?
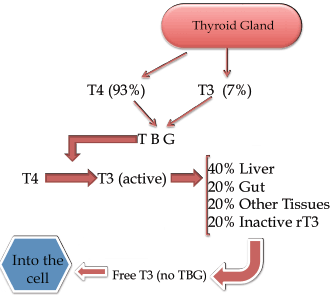
What usually goes wrong in this production process? In the chain of thyroid hormone activity, any point can pose a problem:
- The thyroid gland itself could not be producing enough hormones. This could be down to; a lack of iodine in the diet, an excess of polyunsaturated fatty acids (PUFA) or goitrogens in the diet, previous thyroid surgery, the so-called ‘autoimmune’ condition Hashimoto’s, etc.
- The liver could not be ‘activating’ the hormones (T4 -> T3), due to a lack of glucose/glycogen, an excess of cortisol, liver damage from obesity, alcohol, drugs and infections, iron overload, etc.
- Cells may not be absorbing the available hormones. Cells’ absorption of active thyroid hormone is usually down to dietary factors. Polyunsaturated fats from the diet (or from stored fats being released during weight loss) actually block thyroid hormone from entering cells. Glucose, or sugars in general (fructose, sucrose, lactose, glycogen, etc.), are essential for both absorption and usage of active thyroid hormone by cells.
Thyroid hormone in the cell
Assuming no impediment exists for thyroid hormone production, and it can reach cells, it acts directly and indirectly on the process of respiration in cells – leading to the complete oxidation of glucose (into carbon dioxide). Without sufficient thyroid hormone to ‘uncouple’ the mitochondrial proteins, the respiration process cannot complete and usually results in lactic acid rather than the end product of carbon dioxide.
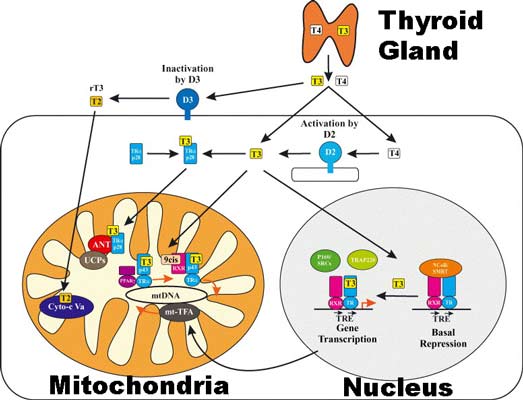
Thyroid hormone acts on both the mitochondria and nucleus of cells, causing short term and long term effects that improve oxidative metabolism. In the nucleus, T3 is thought to influence expression of certain genes, leading to mitochondriogenesis, meaning more/new mitochondria. On the mitochondria that already exist, it exerts a direct energy improving effect via cytochrome oxidase, as well as uncoupling respiration from ATP production.
This means that glucose can be pushed down the respiration pathway without necessarily having to produce ATP. While this may seem wasteful, it increases the amount of beneficial carbon dioxide, and stops glucose being stockpiled as lactic acid. This can be seen more closely in diabetics, who frequently get high levels of lactic acid leading to a state called lactic acidosis. Many hypothyroid people even produce significant lactic acid at rest. Thyroid hormone plays a direct role in alleviating this harmful state.
Thyroid hormone has another function in the body, combining with vitamin A and cholesterol to form pregnenolone – the precursor to all steroid hormones. This means that low thyroid levels inevitably result in low levels of progesterone, testosterone, etc. Low levels of bile salts will also occur, thereby hampering digestion. Thyroid hormone is perhaps the most important hormone in the body, supposedly regulating all essential functions and feelings of wellbeing.
Summary
- Thyroid hormone is considered by some to be the body’s ‘master hormone’ and production relies mainly on the thyroid gland and liver.
- Active thyroid hormone stimulates mitochondrial energy production, formation of more mitochondria, and steroid hormones.
- Hypothyroidism is a state of low cellular energy with many symptoms.
- Causes of low thyroid are complex, relating to diet and lifestyle.
- Low carb diets and high PUFA content in the diet are prime offenders, along with stress.
Thyroid light therapy?
As the thyroid gland is located under the skin and fat of the neck, near infrared is the most studied type of light for thyroid treatment. This makes sense as it is more penetrative than visible red (Kolari, 1985; Kolarova et al., 1999; Enwemeka, 2003, Bjordal JM et al., 2003). However, red as low in wavelength as 630nm has been studied for thyroid (Morcos N et al., 2015), as it is a relatively superficial gland.
The following guidelines are commonly adhered to studies:
- Infrared LEDs/lasers in the 700-910nm range.
- 100mW/cm² or better power density
These guidelines are based on effective wavelengths in studies mentioned above, as well as studies on tissue penetration also mentioned above. Some of the other factors affecting penetration include; pulsing, power, intensity, tissue contact, polarization and coherence. Application time can be reduced if other factors are improved.
In the right strength, infrared LED lights could potentially affect the entire thyroid gland, front to back. Visible red wavelengths of light on the neck will also provide benefits, although a stronger device will be needed. This is because visible red is less penetrative as mentioned already. As a rough estimate, 90w+ red LEDs (620-700nm) should provide good benefits.
Other types of light therapy technology like low level lasers are fine, if you can afford them. Lasers are studied more frequently in the literature than LEDs, however LED light is generally considered equal in effect (Chaves ME et al., 2014. Kim WS, 2011. Min PK, 2013).
Heat lamps, incandescents and infrared saunas are not as practical for improving metabolic rate / hypothyroidism. This is due to wide beam angle, excess heat/inefficiency and wasteful spectrum.
Bottom Line
- Red or infrared light from an LED source (600-950nm) is studied for the thyroid.
- Thyroid hormone levels are looked at and measured in every study.
- Thyroid system is complex. Diet and lifestyle should be addressed too.
LED light therapy or LLLT is well studied and ensures maximum safety. Infrared (700-950nm) LEDs are favoured in this field, visible red is fine too.
Recommended Light Devices
References
ISRN Endocrinol. 2012; 2012: 126720. Assessment of the Effects of Low-Level Laser Therapy on the Thyroid Vascularization of Patients with Autoimmune Hypothyroidism by Color Doppler Ultrasound. Danilo Bianchini Höfling, Maria Cristina Chavantes, Adriana G. Juliano, Giovanni G. Cerri, Meyer Knobel, Elisabeth M. Yoshimura, and Maria Cristina Chammas
Lasers Surg Med. 2010 Aug;42(6):589-96. Low-level laser therapy in chronic autoimmune thyroiditis: a pilot study. Höfling DB, Chavantes MC, Juliano AG, Cerri GG, Romão R, Yoshimura EM, Chammas MC.
Lasers Med Sci. 2013 May;28(3):743-53. Low-level laser in the treatment of patients with hypothyroidism induced by chronic autoimmune thyroiditis: a randomized, placebo-controlled clinical trial. Höfling DB, Chavantes MC, Juliano AG, Cerri GG, Knobel M, Yoshimura EM, Chammas MC.
Azevedo LH, Aranha AC, Stolf SF, Eduardo CD, Vieira MM. Evaluation of low intensity laser effects on the thyroid gland of male mice. Photomedicine and laser surgery 2005; 23: 567-570.
Photochem Photobiol. 2015 Jul-Aug;91(4):942-51. Phototherapeutic Effect of Low-Level Laser on Thyroid Gland of Gamma-Irradiated Rats. Morcos N, Omran M, Ghanem H, Elahdal M, Kamel N, Attia E.
Dubovik V. The postoperative rehabilitation of the autoimmune thyroiditis patients with the use of lowintensive laser radiation.
Photomed Laser Surg. 2014 Nov;32(11):612-7. Effect of three different protocols of low-level laser therapy on thyroid hormone production after dental implant placement in an experimental rabbit model. Weber JB, Mayer L, Cenci RA, Baraldi CE, Ponzoni D, Gerhardt de Oliveira M.
Вера Александровна Кривова: Non-invasive low level laser system in rehabilitation of patients with autoimmune thyroiditis (Диссертация, 2010) – Translated
Д.А. ПУЗИН: Laser therapy in the treatment of subclinical hypothyroidism of various etiologies – Translated
Photomed Laser Surg. 2014 Aug;32(8):444-9. Effects of low-level laser therapy on the serum TGF-β1 concentrations in individuals with autoimmune thyroiditis. Höfling DB, Chavantes MC, Acencio MM, Cerri GG, Marui S, Yoshimura EM, Chammas MC.
J Athl Train. 2004 Jul-Sep; 39(3): 223–229. Low-Level Laser Therapy Facilitates Superficial Wound Healing in Humans: A Triple-Blind, Sham-Controlled Study. J. Ty Hopkins et al.
Rajender S, Monica MG, Walter L, Agarwal A. Thyroid, spermatogenesis, and male infertility. Front Biosci (Elite Ed). 2011 Jun 1;3:843-55.
Kolarova H, Ditrichova D, Waqner J. Penetration for the laser light into the skin in vitro. Lasers in surg Med 1999; 24: 231.
Laser Ther. 2011; 20(3): 205–215. Is light-emitting diode (LED) phototherapy really effective? Won-Serk Kim and R Glen Calderhead
An Bras Dermatol. 2014 Jul-Aug;89(4):616-23. Effects of low-power light therapy on wound healing: LASER x LED. Chaves ME et al., 2014
Irani S, Monfared SSMS, Akbari-Kamrani M, Abdol-lahi M, Larijani B. Effect of low-level laser irradiation on in vitro function of pancreatic islets. Transplantation Proceedings 2009; 41: 4313-4315.
Mendis-Handagama SM, Siril Ariyaratne HB. Leydig cells, thyroid hormones and steroidogenesis. Indian J Exp Biol. 2005 Nov;43(11):939-62.















Would this be useful at all for hypothyroidism induced by part or full thyroidectomy?
Hi Janet.
Interesting question which I haven’t seen any studies on specifically.
Unfortunately, with the total absense of a thyroid gland because of surgery, I can’t see any way in which light therapy could stimulate production of thyroid hormones.
With a partial thyroidectomy only, there is hope. The red light would in theory make the remaining thyroid tissue more effective, though it’s still unlikely to ‘cure’ hypothyroidism alone.
Hi John,
I have Hashimoto’s but have corrected it mostly with diet. I do not require thyroid meds. I do have a large thyroid nodule and of course my thyroid looks like swiss cheese on ultrasound. I do have some lingering adrenal fatigue; never a morning person and feel better at night because my cortisol is reversed. My adrenals do not like anything stimulating like caffeine and anything new in my body usually causes palpitations, basically sympathetic stimulation. My adrenals are so sensitive,
My questions are:
1) would red light and nir be okay for me? I’ve heard that it can stimulate the fight or flight response and I hate that feeling and wouldn’t want to do anything to cause it.
2) Would it help my thyroid nodule shrink?
3) Since I don’t take thyroid meds (my TSH is 2.0, but I do have positive TPO antibodies) could this cause me to become hyperthyroid? Or is it more adaptogen in nature, meaning it only does what your body needs and won’t over correct causing me to become hyperthyroid?
I have heard so many positive things about this therapy that I really want to try it. I would love if it gave me greater energy. I also have bad knees and of course I’d love to use it on my face for cosmetic reasons.
Thank you for your help!
Grace,
What type of food did you eat?
More likely what she didn’t eat. Avoid Gluten, PUFAs, processed foods and sugar. Eat fructose high fruits, himalayan/sea salt, potasium & calcium rich foods. If you can eat eggs and quality meats/fish. Check out the hypoallergenic diet for a list of good and bad foods.
The avoidance of PUFAs seems misguided and misunderstood. PUFAs are ESSENTIAL not optional. However if you are consuming high amounts of omega 6 (usually coming from people who eat lots of processed foods containing lots of vegetable oils such as canola, palm, corn soy OR you have eaten animals that were not grassfed but instead ate high omega 6 vegetables such as corn, soy etc.) this can actually inhibit your ability to process omega 3 which is extremely beneficial to the brain as well as being the vehicle that transports other nutrients such as CALCIUM to where it needs to go in the body. So if you are eliminating PUFAS how is taking in more calcium going to help if theres no ESSENTIAL FATTY ACIDS to transport it?? Also you dont want to just eat “quality” eggs, meat, fish because what does this mean? More specifically you want to eat at the very least animal products from animals that were pasture raised(another vague term) and at best are 70-100% grassfed and finished. This includes farmed fish because they are now fed corn and soy effectively eliminating the high omega 3 benefits of fish. We all have to become more specific in what the dietary issues are because while you could up you carbohydrate intake by eating white bread, fruit seems obviously a better choice.
The original studies (Burr et al.) establishing the ‘essential’ nature of some PUFAs (inc. Omega 3) are now known to be flawed. Using special diets devoid of vitamins they didn’t know to exist at the time (1929). Claims about Omega 3s being good for the brain, heart, eyes, etc., are debatable at best, with mixed evidence and disputed mechanisms.
Given that the Cyclooxygenase group of enzymes in our bodies convert PUFAs into pro-inflammatory prostaglandins, it makes sense to be somewhat sceptical about them.
Please clarify what this PUFA acronym means. Thank you.
Polyunsaturated fatty acid.
I am trying to avoid surgery. What diet did you follow that corrected it? Do you have water that is fouride treated or well water? Thank you. Lisa
1) It should be fine. Light therapy only restores your normal respiration.
2) Unknown, possibly.
3) I guess adaptogen is the right term, yes. It alleviates stress, it doesn’t stimulate beyond what is normal.
Iodine will shrink the thyroid nodules and breast, The fda levels should at least equal the bromine amounts they stick i everything
Which device should I purchase for autoimmune induced hypothyroidism?
I have Graves’ disease can red light be beneficial for me?
I am not sure that I have seen light therapy studies specifically on Graves’, so it would be hard to make any definitive statement. I have seen studies on other autoimmune issues where the light therapy was considered to give a beneficial effect.
What about the tanning beds that offer red light therapy? Would that be the same kind of light?
It’s hard to find technical information on those red light therapy ‘tanning beds’ and their bulbs. Without information on wavelength and light output, you can’t calculate the time required for a good dose.
The way they’re marketed (‘boost collagen production!’) just isn’t true, and there may be a negative effect of EMF exposure from being inside a 2000w+ machine.
Having said that though, they obviously do emit red light of some sort, so I believe they are beneficial. I’m not sure that they’re suitable for thyroid treatment specifically (the strength of red light used may or may not penetrate the skin), but they should provide an anti-inflammatory effect which may indirectly help hypothyroidism or general health.
With regard to chronic dry skin therapy, the Red light device product page says:
“Do not position the light directly in front of the eyes for extended periods, even with eyelids shut.”
What if the affected area is basically all of the skin surrounding the eyes? What to do then?
Hi Phil, yeah good question. You can use some tanning goggles to fully cover the eye balls but without covering much skin in that area. Just search on amazon or google for ‘sunbed goggles’ or ‘tanning goggles’.
Hi!
Very interesting article and product! I will be saving my pennies in hopes of purchasing one soon.
Thanks for the info!
Glad to see this site up. And extra points for being in the UK! About the only Peat approved health supplement I won’t need to pay a bazilion pounds extra on shipping for :s
Would this be beneficial for Hashimoto’s?
Some of the studies referenced above were on people with hashimoto’s. The Höfling et al studies reported a reduced count of autoimmunity markers, as well as a reduction in the dose of T4 required by patients.
I’m wondering what effect red light might have on connective tissue like collagen in general
I don’t think red light interacts with collagen directly in any way. Collagen is a hard protein deposit that is mostly void of metabolically active cells.
Red light has been shown to affect cells that produce collagen (such as osteoblasts in bones, and fibroblasts in skin and joints), normalising collagen production there and potentially reducing the formation of scars during healing, and perhaps preventing wrinkles over time.
Red light therapy at 660 nm is suppose to build the collagen so it has anti-ageing effects. justluxe.com/community/21-proven-benefits-of-red-led-light-treatment_a_1769088.php
That’s the way most marketers explain red light and collagen, but I think it’s a lot more complicated. Simply ‘building collagen’ is actually associated with scars, wrinkles, fibroids and even some tumours.
It’s better to say that red light normalises collagen production, helping cells to find the balance between new collagen production and old collagen breakdown – keeping skin soft and flexible.
There is more info here – https://redlightman.com/health/collagen-light-therapy/
Have people used red light devices with success in warming their extremities? I often have cold hands and feet which I believe is connected to thyroid/metabolism issues.
These light therapy devices are low power, not very heating generally. You’d be better off getting some radiant room heaters. Also addressing the thyroid problem itself as discussed on this page.
Look into the Sauna Space single bulb (or full sauna/panel). It is a full spectrum red light, NIR and FIR bulb that produces heat in addition to the infrared therapy benefits. It is what I use, and I love it.
Heat isn’t an ‘addition’ to light therapy, but something that cancels out the benefits of it, and should be avoided. Broad or ‘full spectrum’ should be avoided too, since the IR-A, B and C infrared wavelengths are absorbed by water molecules in our skin, leading to a heating effect..
You can argue that skin heating (above normal body temperature) is good in certain situations, like if you are cold, or the detox/sweating mechanism, but metabolically it is definitely not good:
https://pubmed.ncbi.nlm.nih.gov/2462905/
Heat denatures our cellular enzymes, including the Cytochrome C Oxidase enzyme via which light therapy works. So heat lamps (or sauna bulbs) prevent the light therapy (a.k.a photobiomodulation, formerly known as LLLT) effects.
So, you haven’t been getting any light therapy benefits whatsoever from that.
Thanks for the article.
I look forward to experimenting with red light to improve my thyroid function.
Fantastic Information. I really need to try one of these lights out. Do you suggest a combo light for the thyroid treatment (like the red/infrared combo)? Or just infrared? Thank you!
Hi Lindsay,
I don’t suggest any medical treatment. In the studies they chose near infrared. Infrared would be perhaps more efficient for reaching the gland.
I notice that some of your lights aere out of stock. When do you anticipate their availability? Also can your units be used in the US?
Just a temporary issue Suzie, should be back within a couple of weeks max. All of our products can be used in the US
This is somewhat off topic, but I am wondering if infrared light is safe to use over a mole? I can’t seem to find info elsewhere. I’ve been using infrared light on my face for anti-aging and it seems to be working already. My skin is softer and my lips look fuller. But, I have a mole just above my lip and I’m wondering if the light will enlarge the mole- I definitely don’t want that.
Hi Amanda,
I’m really not sure about that. I haven’t seen any data regarding moles and red or infrared light.
All I can say is that I have a couple of moles on my face and after years of using light I have not noticed any interaction. It’s not something I’ve ever had a reason to worry about.
Hi,
Can I use the cheap ones like Infrared Light Device Mini for boosting metabolism? I can’t afford the ~200 eur one right now.
Would it be a matter of applying it more time?
Thanks
Hi Marcus,
Yes of course. You can get all of the same benefits in theory. The beam on our smaller lights (vs bigger lights) just covers a smaller surface area.
Thanks Joe! That’s great news 🙂
By the way… Are you aware of any specific benefits of applying it to the liver area? Scientific studies or testimonies.
Thanks!
I haven’t seen anything studying that specifically in humans. It should have the same effect in liver cells as elsewhere in the body though. All cells need energy. You would need a large dose to get any direct effects in a deep organ like the liver though.
I saw a rat study once which noted liver regeneration after surgical removal.
Hey John
Thanks for your post! It looks like you are suggesting to use LED lights (as per post/research above) but what about a near infared bulb? I don’t think LED gets warm — but I know the near infared does. I want to use it to reduce/eliminate/heal thyroid nodules. Have you come upon any research about that? And which bulb? Thanks!
Hey Ellen,
If you’re talking about the 250w heat lamp type bulbs, I’ve done some tests on them with solar power meters to estimate power density of 600-900nm light (by factoring in the overall spectrum). You have to use them from about 10-15cm to get a good power density (100-200mw/cm2) of the 600-900nm wavelengths.
Unfortunately at this distance, they heat my skin pretty quickly and it is painful. After doing those tests, I think they’re pretty useless for the purpose of light therapy. I don’t think it’s possible to build up high doses or get the high power densities that you need hitting the skin (at least without burning your skin) for deeper penetration.
They are mainly useful just for heat, if you are cold in winter for example, and keeping warm has its own benefits, but due to the broad spectrum, prolonged use will contribute to skin photoaging quite significantly. It’s not a light therapy product in my opinion.
Hey Joe
Thanks for your reply. If you look on amazon for nir-a near infrared bulbs by rubylux you’ll see that people dealing with cancer and other aches and pains and inflamation use the near infrared bulb for spot treatment to heal and detox. I think I’m going to try it out, was just looking for some studies or testimonials for thyroid node reduction/elimination by using this. Btw, if it’s too hot, I would just sit further. It’s supposed to make you sweat out toxins.
Good luck with that Ellen. It looks like a standard heat lamp bulb. It should be ok as far as heat therapy goes. I wouldn’t expect any effects on the thyroid directly though as the light won’t be able to penetrate that deep in sufficient doses.
How frequently should you use the infared light on your thyroid? Can you over do it?
I would not make specific recommendations for things like that. For light therapy in general 3 times per week is a good base. Nothing bad will happen if you go crazy with it, although the benefits may be diminished or gone.
Been reading on raypeatforum about your products because I have heard you’re the best. Looking forward to using it on my Hashimoto’s condition.
I’m looking to use this for thyroid function but am not sure if my thyroid is actually an issue (but I suspect it could stand for improvement). Which light would you suggest?
Most of these studies referenced used 830nm light. I however would not recommend any medical treatment.
Hi, thanks so much for all the great info on this website. Very informative and helpful! What are your thoughts on people using LED security illumination devices (like the ones used for CCTV)?
The wavelengths are usually off for light therapy (ie 850nm instead of 830nm) and you’ll need to get some sort of irradiance power meter to measure the output (and how the output changes by distance).
Do you have any that are less expensive that would work for my thyroid? Anything cheaper than $200?
I would not make medical recommendations like that.
What’s the difference between your product and an LED light? I’m using an LED light with the correct wavelength and not seeing any difference.
Our products are LED lights. With lights in general, wavelength is one thing, but power density is more significant. If you are just buying a random LED light intended for other purposes, you won’t know the power densities, and even if you did, they are probably way out of the appropriate light therapy range.
Joe, I’m not sure that one can know where the process of the thyroid system may have broken down so with the light therapy one is first attempting to heal the thyroid to see if that is the weak link in the process. Yes? But if there is a weak link somewhere else in the system then what is the next step? Or can light therapy on the thyroid heal the whole system?
Hi Rex, you may also want to address leaky gut, toxins, or other infections. I think once you’ve done all this as well as this therapy you might be able to put the disease into remission. It has to be a multi-pronged approached.
To our health,
Vanessa
Rex, if your hypothyr is the result of pituitary unable to produce enough TSH, or reduced liver conversion of T4 to T3, then lighting the thyroid isn’t going to help. But most people have “primary hypothyroid” (with high TSH and low T4) and that may benefit from healing the thyroid. First get the TSH T4 and T3 tests which the nhs will do free if you nag them enough with moans about your lack of energy etc.
Hi Joe, do you have a protocol to apply this to the thyroid? Also, have any of your past customers reported their results? Have you seen varying results from the mini vs the larger model.
Has laser therapy been shown to help with low testosterone production?
In animals there is a lot of data, yes. I haven’t seen much in humans, but since testosterone production is downstream from thyroid, and light therapy may potentially aid the thyroid, you can assume it helps downstream.
Hi Joe,
Some users on the RP forum, including myself, have reported a strange and uncomfortable throat pain/sore throat on the thyroid area when using red light on the thyroid. I’m using the red light mini for instance. Just a couple of examples :
“- had the scratchy throat feeling but I can’t explain it. It didn’t stop me and it went away, was never painful at all just a bit weird.”
“After a few minutes my throat felt very uncomfortable on the inside, like I was beginning to get a sore throat, it felt almost hot and dry on the inside. The light itself wasn’t hot and my skin wasn’t red in any way, it was on the inside. It wasn’t a pleasant feeling and I stopped, the rest of the day my throat felt slightly raw, back to normal the day after.”
This is also happening to me. What do you think is this ? Have you had other users reporting this ? Should I be worried ? I don’t think I overdone it. It started to happen to me after a couple of days doing it 2 times x day, 10-12 minutes each. Is this too much ? I’m a bit scared.
Hi Marcus,
It sounds like a psychosomatic response. The throat is actually one of the main areas that feels weird during anxiety. You can see by searching online that people with various anxiety issues get a similar sort of burning throat, lump in throat, tight throat, etc. I am especially confident of this considering that you are using the red mini. Given the penetration of red light, it won’t be having a significant effect on areas deeper inside the throat and thyroid. Red is more for skin, near infrared for deeper penetration. So actually having a direct sensation in areas that the light won’t even penetrate to is definitely just a nocebo/anxiety type of effect.
I don’t mean to dismiss those anecdotal experiences. I suppose it is possible that there could be something going on, like some minor local vasodilation from the CO2 production and NO release, which is just a short term minor issue, nothing serious. It is more likely just a psychosomatic response from the way you are positioning the neck during the sessions and the mental focus on that area, plus the negative expectations.
I don’t think you are doing it ‘too much’ with your sessions, but the studies I have seen used it less frequently. I believe only once per week in one. I think every other day is enough for 5-10 minutes.
Hmmm thanks a lot for the detailed answer Joe. The penetration thing makes sense. Anyway I have had those “lump on the throat” feelings you mention on the past due to anxiety and this is very different. I remember having them also while using high dose iodine in the past. It’s different than this. This is more like… if you smoke a LOT of tobacco, something like “irritation”. I will let you know how it goes when I experiment more anyway. It could be useful for other people. I’m very happy with the light anyway. Thanks again!
I have had this side effect as well. My unit has both red and infrared settings. Very dry, feels scratchy or swollen. I used infrared and red for only two minutes six inches away, then red on whole upper body for 3 minutes, farther away. And this happed. Went down to one minute on infrared six inches away only, then 3 minutes farther away red only. I have only done this three days in a row, so may do no more thyroid, only red light farther away for another day. Am thinking five days/week or six, but less on intense thyroid. Marcus, did you continue to use this?
Every time I use laser on my thyroid, I have discomfort, a feeling of swelling and just not a pleasant feeling. I think if you react this way, it’s wise to listen to your body and not push it. Or try it at the back of the neck perhaps.
You stated red is more for the skin, and infrared would penetrate deeper, but I thought the light therapy is infrared?
You stated red is more for the skin, and infrared would penetrate deeper, but I thought the light therapy is infrared?
to Marcus -Did you continue using the light, did it help your thyroid?
Hi Joe. Is there a particular clip on bulb holder or flexi-neck desk lamp that you recommend for the red light and infrared minis that you sell?
Hi, it’d be interesting to see a chart of all the conditions you cover on your blog showing whether the visible red or infrared is better to help people decide which light to get.
It is pretty simple, due to the penetration difference. Red light does not penetrate as deeply as near infrared.
So red light would reach surface tissues.
Near infrared light is for everything else (deeper tissues)
Hi. I have the full body red light combo device. What kind of treatment would you recommend for the thyroid using said device? I only ask because due to the fact that it covers the entire body I thought that perhaps it is different and less time is needed due to the systemic effect of the light on the whole body. For example, 10 minutes at 10cm 3 times a week or is this too much? Also any thoughts on how long for hair loss? By the way LOVE the product have had a number of health benefits already from use. Also I have a friend who used it and said their anxiety almost disappeared instantly and they had the best sleep ever. Also someone who has Parkinson’s disease who said they felt a beneficial effect.
Thanks for the feedback Soren, very interesting. The benefits seems to hold true for a wide variety of health issues.
For general use, I would recommend using it from about 50cm away, for 10-15 minutes.
I would not make recommendations for specific medical issues.
What would light therapy do for someone with overactive thyroid disease? Reading this article makes me think it would make it WORSE if it increases thyroid hormone.
Light therapy doesn’t necessarily increase thyroid hormone. The mechanism of action is that it simply ‘resets’ your cellular energy production. So for people that have a weak thyroid, light therapy might brings those thyroid gland cells up to normal. For people with overactive thyroid, it might also just restore normal function.
I would like to buy the “Infrared Mini Light Device” to treat my chronic autoimmune thyroid disease. I know that you have answered this question a lot of times, but it’s difficult to understand for me:
1) What distance would you apply the light for the thyroid gland therapy?
2) How long? (with your “infrared mini light device”)
3) How many days a week you would apply the light therapy?
Thanks very much! I’m very interested in your product.
To give deeper tissue in general a reasonable dose of light, I would apply a suitable device from fairly close, maybe 10cm away, for 5-10 minutes. Some people have mentioned longer doses (15 minutes twice a day) as being great for them.
I’ve been reading conflicting information on red light therapy. One study was done on rabbits, and it showed the opposite of helping the thyroid. Do you know anything about this?
No….but I have seen thyroid studies on rabbits too and they were beneficial. I remember one indirect study, using light on the teeth/gums of rabbits and monitoring T3 active thyroid hormone levels and they improved. So improvements even without direct thyroid gland treatment.
Based off this information, what is the dosage time, and distance you would suggest when using your near infrared light bulb mini, to replicate the results of the studies?
10-15cm distance for 5-10 minutes.
Hello, I am so interested in trying this! I have both graves and hashimotos autoimmune thyroid disease with a large goiter and currently being treated with methimazole to bring the thyroid levels down. Do you know of any studies of the near infrared light therapy for my situation or for hyperthyroid issues? Thank you!
Yes, check out some of our referenced studies above.
Hi Joe,
based on the studies outlined and your own experience would the infrared light 830 device be most suitable for raising low metabolism? if so, how long for, how often and how close to the target gland (I.e thyroid) would you recommend
thank you
Yes, the studies I have seen and experience indicate the 830nm range. I cannot make direct medical recommendations. Studies I have seen on the topic indicated a low or high dose were both effective.
Hi,
Just want to share my experience. I bought a combo mini from Joe about a year ago, for general use, muscles when training, skin treatment, both anti-aging as well as for cuts. But in August last year I had a blod test done, which showed a too high TSH of 5.2, although T3 and T4 still normal (I re-checked old tests and realized that I had a TSH at 3.7 already 2012, but no one, including me, reacted then). With these values, and without obvious symptoms, am I not seen as having an illness, yet. I checked the research, specifically Löfling Joe is referencing, calculated the energy to know for how long I would use my lamp, and at which distance, to get the same light effect as they were using. Then I followed their protocol of twice a week treatments, 10 times. Three months later I re-took the blood test and had a TSH of 3.6, still not perfect, but in my opinion clearly showing that the treatment works. I will continue my treatments, and check at times, and I hope, and slightly expects, to get back to “normal values”, below 2, as I believe that values above 2 is not optimal.
I believe however that it is of outmost importance to do your math in these things, just random treatments without calculating the J/cm2 do I not believe in.
I feel very encouraged and will buy another device as well.
Regards
Lotta
What was your protocol?
Hi I have hypothyroidism with TSH of 5.2, I want to try your products pls send me the details
Narendra, I think you have to scroll up to the top of the page and click on the products link to get information about them
In the article it gives the wavelength but not the dose. What would the dose be for the hundred megawatt per cm2 machine?
Hello! Wich device would be best to buy for Hypothiroide and general higher vitality? The combo? or a smaller one? And how long & range would be a good advice to try? thank you!
The studies I have seen on hypothyroidism looked at the 830nm wavelength.
The range of doses that seemed effective (according to the studies) varied, from low doses to high doses.
Hi,I am on 175 mg of Levothyroxine, underactive thyroid,can I use led light therapy ?
Hello, I am a female, 63 years old, and was diagnosed with hypothyroidism when I was 30 years old. I have always been overweight. And almost every time I have a blood test i have to increase my dose of meds. I am up to 325mcgs. I also have MS so I am always tired from both illnesses.
My question for you is, I bought one of those Red light therapy for face and neck. It has the blue, green, and red light, the red light strength is the highest at (620nm-630nm) . Do you think it’s strong enough to help me if I used it over my thyroid? and for how long? It says don’t go over the middle of the neck with it, so that why I looked it up and found your website with tons of great info, thank you. if not what kind of light do I need ? Thank you for your time. Sincerely, Dana
Hi Dana, I’m sorry to see no one has responded to your comment. And I’m sorry for your struggles. I also have hashimotos. I’ve had it for about 10 years. I just reluctantly started medicine again after being off for a few years, because it never made me feel better before. I had forgotten about infrared light therapy but have been researching for about 6 hours today. I’m so happy I stumbled onto this website. I’m about to buy Joe’s 830 near infrared fully body device. This is what you would need for your thyroid too (830 infrared, not necessarily the full body). The device you mentioned with the red wavelength at 630 would not penetrate deeply enough to reach the thyroid and provide any benefit. It would only provide surface level, skin benefits. This site is definitely the best in terms of staying true to the efficacy from proper irradiance found in the research studies. So many of these other companies are just marketing and providing cheap bulbs. If you’re still interested in exploring healing your thyroid with infrared light, I would recommend 830 infrared found on this site. I’m not an affiliate just a very passionate consumer.
Is it safe to use DPL lights multi color if you have thyroid nodules or goiter?
Many thanks for any information you can share.
I am interested in treating hair loss and low thyroid. I asked what advantage the $260 product has over the $156 one which looks as though it gives more coverage. Ari Whitten has said to get a 670 device.
Can you toggle between nm on the combo mini or does it just use all nm all at once? Which device allows you to choose red light or nir or both? Thx
Can infrared light therapy help with kidney disease?
Hi Joe,
I have a high TSH and nodes on my thyroid.
I do have your device 830.
How should i use it to treat my thyroid please (what the distance from a thyroid, how many minutes, how many times per week and how many times in total)
Thank you.
How long and how often should one use the light assuming using something like the full body model? I know there are variables as to distance and light strength and I’m studying those.
However I haven’t seen a dosage recommendation. Need not be specific simple guidelines would be greatly helpful. Thanks
Hi there, I have managed to bring down my levothyroxine meds from the prescribed 75mg to 25mg over 6 months of using my red light (infrared small cube one) I just had a blood test and my T4 levels are now normal, I am so delighted. I want to keep doing it until I wean myself completely off the mess. Question: I have been using my light most evenings for 12 minutes, close to my thyroid, I am wondering if I can use it and leave it on during a 30min meditation, what distance would be recommended for this? Thanks in advance, Ellie
Ellie, do you also have Hashimoto’s? How long have you been on your meds for?