General Wellbeing, Health, Light
Red Light and Yeast Infections
Light treatment using red or infrared light has been studied in regards to a whole host of recurrent infections all over the body, whether they are fungal or bacterial in origin.
In this article we’re going to look over the studies regarding red light and fungal infections, (a.k.a. candida, yeast, mycosis, thrush, candidiasis, etc.) and related conditions such as vaginal thrush, jock itch, balanitis, nail infections, oral thrush, ringworm, athlete’s foot, etc. Does red light show potential for this purpose?
Contents
Introduction
Can Light Therapy Reduce Inflammation
Red Light Helps Kills Yeast?
Possibly Solving Recurrent Infections with Light
Summary
Recommended Products
References
Medical & Healthcare Disclaimer
The information contained in this article is not intended or implicitly suggested to be an alternative for professional diagnoses, or profesionally recommended treatments & medical advice. Absolutely all of the content, including the article text itself, images, comments and other information, contained on this web page is for non-specific information purposes only. We strongly suggest that one should never ignore professional health/medical advice and we strongly suggest that one must not delay seeking a professionally recommended medical treatment because of information attained via reading this article/website. The products sold or recommended on this web site are absolutely not for the diagnosis, prevention, monitoring, treatment or alleviation of any specific disease, injury or disability.
Introduction
It’s surprising just how many of us suffer from chronic infections on a weekly or monthly basis. While some may write it off as a part of life, inflammatory issues like this are not normal and need to be treated.
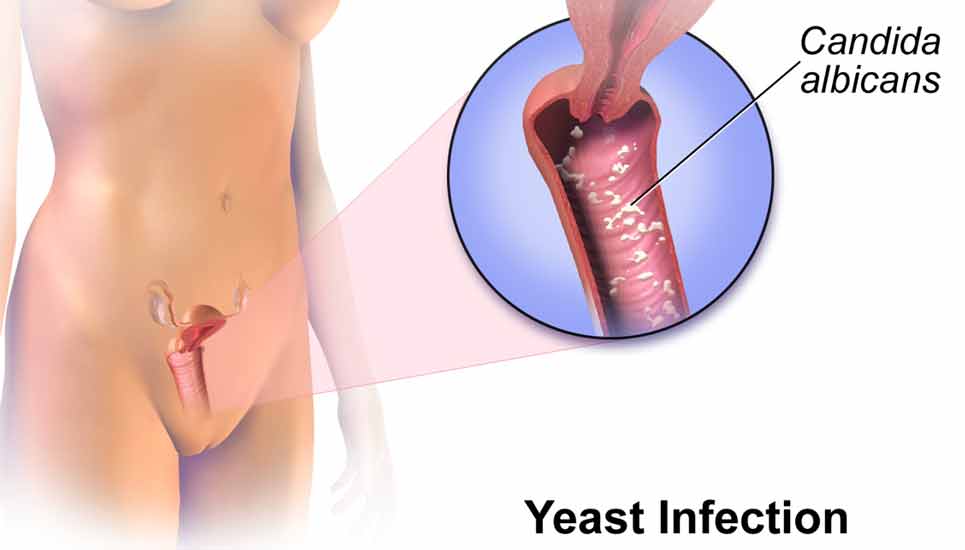
Suffering from recurring infections puts the skin in a state of constant inflammation, and in this state the body forms scar tissue rather than healing with normal healthy tissue. This disrupts the function of a body part forever, which is a major problem in areas like the genitals.
Whatever and wherever on the body you might be prone to these issues, it’s likely that red light therapy has been studied.
Why exactly is red light of interest in regards to infections?
Here are a few ways in which light therapy might help:-
Red Light Reduces Inflammation?
Redness, soreness, itchiness and pain are typically linked to infections, as the immune system tries to defend against the aggressive microorganisms. The stress of this interaction on the local tissue contributes towards increased inflammation, which contributes to fungal growth. Many prescriptions and creams used for treating infections contain anti-inflammatory compounds like hydrocortisone. These can help the body to deal with the stress, but some say this just masks the underlying problem.
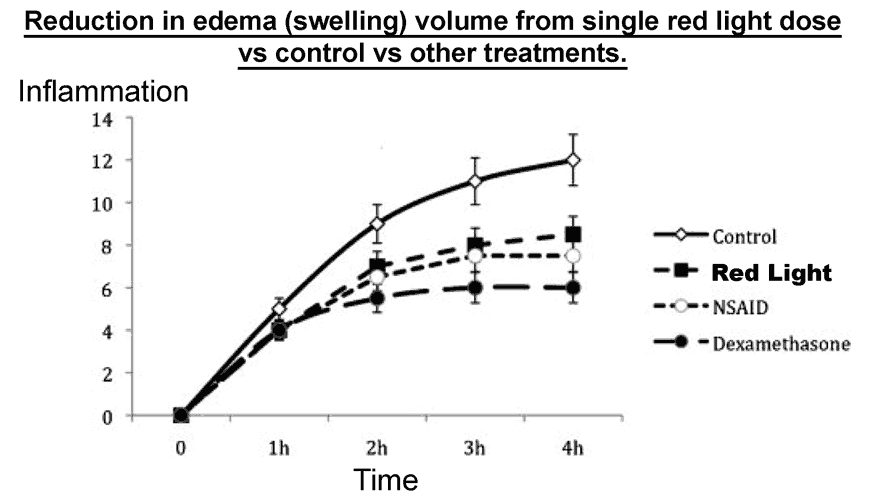
Some studies on red light lead to the potential conclusion that it may actually help the body to deal with the metabolic causes of inflammation5, allowing cells to produce more ATP and CO2 through our normal respiration reaction. These products of respiration have a supposedly almost identical effect to anti-inflammatory compounds in that they inhibit prostaglandin synthesis (prostaglandins being a main mediator of the inflammatory response) and stop the release of various inflammatory cytokines.
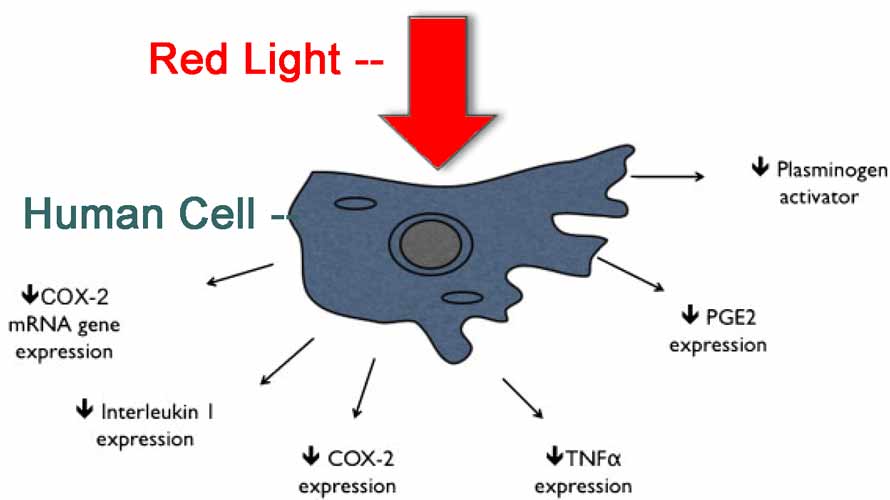
Some people think inflammation is a necessary part of the healing response to infections or injury, but it should be considered a symptom of the body not working correctly. This can be shown by how in the fetus of most animals, it’s normal for an injury to heal without any inflammation whatsoever, and even in childhood, inflammation is minimal and resolved quickly. It’s only as we age and our cells stop functioning properly that inflammation increases and becomes a problem.
Light Therapy harms Yeast & Bacteria?
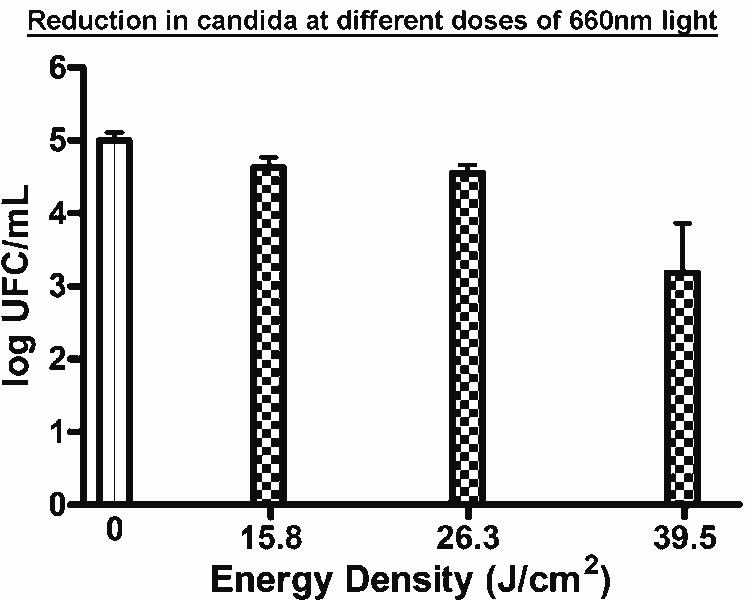
Perhaps the main reason behind the interest in red light for infections is that red light can, in some organisms, directly destroy the fungal or bacterial cell body. Studies show a dose dependent effect, so it’s important to get the right amount of exposure. It seems that in the studies done on the topic, higher doses and longer exposure times eradicate more of the candidaFIG 2. Low doses seem to just inhibit the growth of yeast.
Fungical treatments involving red light usually also involve a photosensitizer chemical, in a combination therapy known as photodynamic therapy. While adding photosensitizer chemicals such as methylene blue does improve the fungicidal effects of red light, red light alone still has an effect in some studies2-3. This could perhaps be explained due to the micro-organisms already containing their own endogenous photosensitizer components, which our human cells do not. The red or infrared light supposedly interacts with these chemicals in the fungal cells, causing a destructive chain reaction that ultimately destroys them.
Whatever the mechanism is, red light therapy alone is studied for infections from a wide range of fungi and bacteria. The beauty of using red light to treat infections is that while the micro-organisms are potentially being killed/inhibited, your own skin cells are producing more energy/CO2 and so inflammation could be reduced.
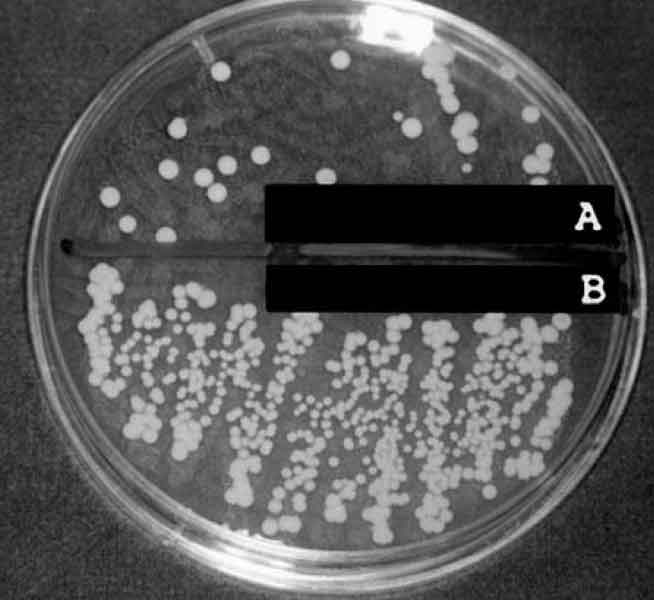
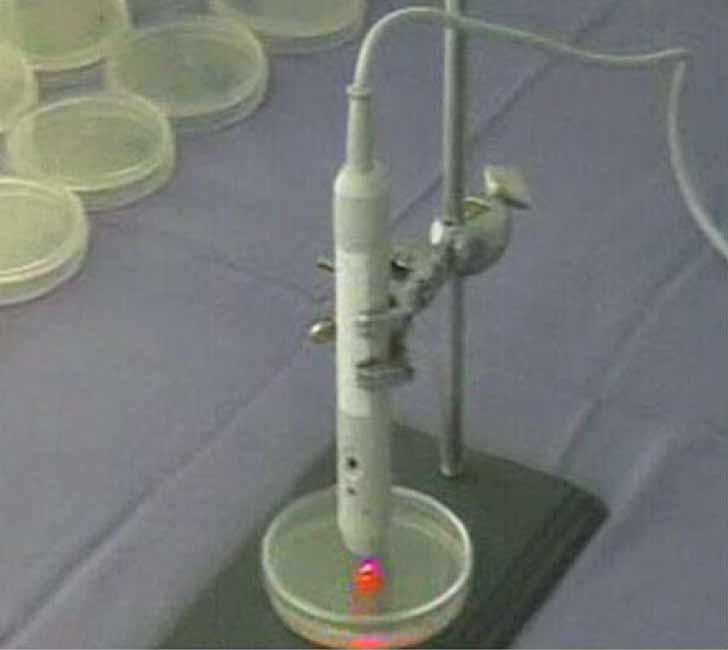
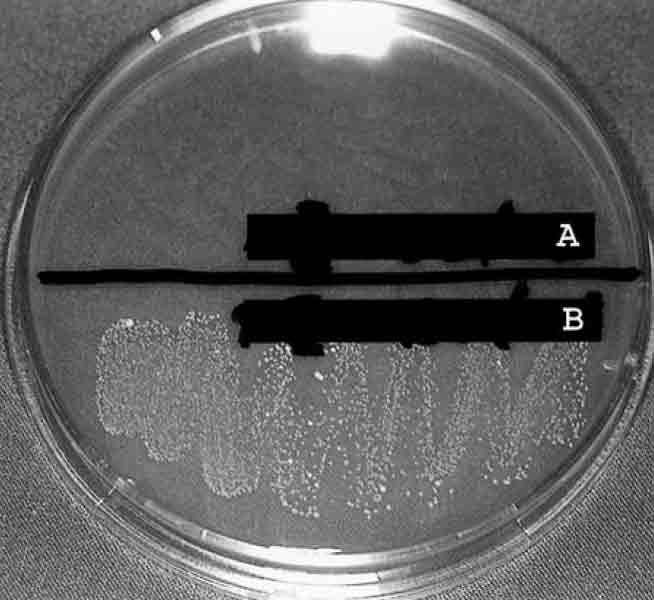
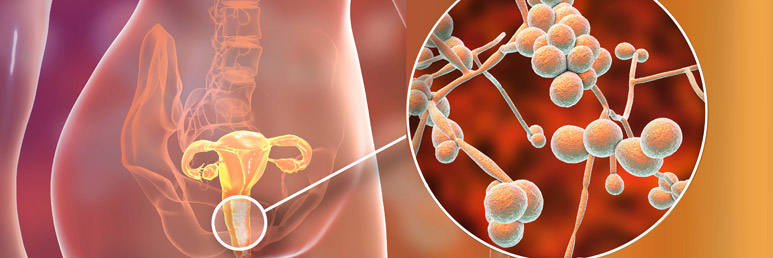
Fig 3. Yeast cells growing on a nutrient plate. Red light being used to kill yeast in the lab at 685nm1-2.
Solving recurring & chronic yeast infections?

Many people experience relapses and recurrent infections, so finding a long term solution is crucial. Both of the above potential effects (healing without inflammation and sterilising the skin of harmful micro-organisms) of red light may lead to a downstream effect – healthier skin and better resistance to future infections.
Low amounts of candida/yeast are a normal part of our skin flora, usually causing no negative effects. Low levels of inflammation (from any cause) actually promote the growth of these yeast organisms specifically, and then the growth leads to more inflammation – a classic vicious cycle. The tiny increase in inflammation quickly esclatates into a full blown infection.6
This can be from hormonal, physical, chemical, allergy related, or various other sources – many things affect inflammation.
Studies have looked at red light to directly treat recurrent thrush infections. It is noted that using red light when you feel a infection coming on is perhaps the best idea, literally ‘nipping it in the bud’. Some research speculates on that idea of using red light consistently over weeks and months to prevent the yeast infection/inflammation entirely (thus allowing your skin to fully heal and flora to normalise) is perhaps the ideal long term solution. The skin in commonly infected areas needs several weeks without any inflammation to fully heal. With the natural structure of the skin restored, resistance to both inflammation and future infection is massively improved.
What type of light do I need?
Nearly all of the studies in this field use red light, most commonly in the 660-685nm range. Several studies exist that use infrared light at wavelengths of 780nm and 830nm and they show almost identical results per dose applied.2
The dose of red or infrared energy applied seems to be the main factor to consider for results, rather than wavelength. Any wavelength between 600-900nm is studied.
With the available data, it seems like appropriately used red light gives slightly more anti-inflammatory effects. Infrared light may give a slightly greater fungicidal effect. The differences are only slight though and not conclusive. Both have a strong anti-inflammatory/fungicidal effect. Both of these effects are equally essential for resolving fungal infections.
Infrared has better penetration properties than red, which is worth noting in regards to deeper fungal infections in the vagina or mouth. Red light may not physically be able to reach candida colonies further inside the vagina, whereas infrared light may. Red light seems interesting for all other instances of fungal infections of the skin.
How to use it?
One thing we can take from the scientific data is that various studies point to higher doses of light as useful in eradicating more of the fungal infection. Consequently, longer exposure times and closer exposure therefore leads to better results. As the fungal cells directly lead to inflammation, it follows that, in theory, higher doses of red light would potentially resolve the inflammation better than low doses.
Summary
- Light therapy is studied for short and long-term treatment of fungal issues.
- Red & infrared light are both studied.
- The fungi are killed through a photosensitive mechanism not present in human cells.
- Inflammation is reduced in various studies
- Light therapy might be used as a preventative tool.
- Higher doses of light would seem to be necessary.
Recommended Products for Yeast Infections
References
- Effect of low-level laser therapy on Candida albicans growth in patients with denture stomatitis. Maver-Biscanin M. 2005
- Effects of low-level laser irradiation on the pathogenicity of Candida albicans: in vitro and in vivo study. Seyedmousavi S. 2014
- Comparison of the photodynamic fungicidal efficacy of methylene blue, toluidine blue, malachite green and low-power laser irradiation alone against Candida albicans. Souza RC. 2010
- Antimicrobial photodynamic inactivation inhibits Candida albicans virulence factors and reduces in vivo pathogenicity. IT Kato – 2013
- The anti-inflammatory mechanism of low level laser therapy and its relevance for clinical use in physiotherapy. Jan Magnus Bjordal. 2010
- Inflammation and gastrointestinal Candida colonization. Carol A. Kumamoto. 2011
- In Vitro effect of low-level laser therapy on typical oral microbial biofilms. FG Basso. 2011
- Treatment of oral candidiasis with methylene blue-mediated photodynamic therapy in an immunodeficient murine model. MC Teichert. 2002





Do you use externally in abdominal area for recurrent yeast infections? Please describe exacxtly how to use for this!
Hi Alice, I think it is more suited for yeast infections near the surface of the body. Like nail infections, outer vaginal yeast, under the foreskin, mouth candida, nappy rash, etc. You could try the more penetrative infrared wavelengths for yeast in the gut, but I think you would require a very large dose to see any effect that way.
Is there one available for yeast infections inside the body? Which one would be used and how?
Yeast infections inside the body (such as small intestines) would be hard to reach with red or near infrared light. This is my recommendation: https://redlightman.com/product/infrared-830-device/ due to the high intensity of penetrative light.
For treating bugs in the gut, roughly how many minutes per session would you recommend on the bodylight combo 2.0 from about 20cm away?
While I would not necessarily recommend that, studies point to the fact that for deeper issues or systemic healing you need quite high doses. This means close exposure or long sessions. I’m not sure the light will get down into the deepest areas of the gut, if any can.
Is this safe for a kitten with ringworm?
Which light and parameter needed to kill ringworm in joch itch ? Also in the surface of vulvar area?
https://redlightman.com/product/red-670-light-device/ ideally, or other red lights, used at a range closer than 8 inches or around 5 minutes, daily.
https://redlightman.com/product/red-670-light-device/ – a session of 3-5 minutes, from 15cm/6in distance, once a day should work.
Where can I purchase a Red Light for chapped lips and broken corners of my mouth? I sure hope you can help me.
Shorter wavelength lights are more suitable for this as there is less absorption by water (less drying effect) in your skin. You don’t want to make the dry skin worse. A product such as this 620nm has utility – https://redlightman.com/product/red-mini-620/
Can you use on different areas of head to effect changes in the brain post traumatically? What times are indicated, and spaced in what way? Every other day, daily, etc., for 2 min.?
Infrared light (810-850nm) has been studied for traumatic brain injury, although I do not specifically make medical recommendations. Red and infrared light seem potentially useful for wound healing on other areas of the body so it makes sense that the same would apply to brain damage. I think you would need a large dose of infrared (dose = power density x time), rather than any specific time, just to make sure enough total energy is getting into the brain. Maybe 100 J/cm2 is a good dose to start at, directly over the part of the brain with trauma. Every day is fine. Twice a day is fine.
I have a reoccurring ear fungal infection and I was hoping to use infrared light to heal and prevent. Do you think this would be safe?
With an appropriate near infrared light therapy device, there is no potential for harm by using it on the ear, so yes.
Did this work for you? Still recurring?
What about shining it on different body parts affected by disease, such as arteries, joints, heart, organ systems? What would the prescribed doses and frequency be?
While I do not make medical recommendations, studies on light indicate that it might help with some symptoms all over the body. You could see a reduction in inflammation (via the increased CO2 from respiration inhibiting the prostaglandins/cytokines pathway), and a improvement in healing due to having more cellular energy. The doses basically depend on the depth of the tissue in the body, with deeper tissue requiring a larger dose. Red light might reach a near surface artery in the neck or arm/foot. Infrared is going to be better if you want to reach organs and large joints. You will need an infrared light that can reach at least 200mW/cm2 power density for that deep penetration too.
Could a red laser (laser pointer) effectively be used for this treatment? I’m trying to clear up ringworm on two rescue kittens. I have anti fungal medicine from their veterinarian and would be using the red laser as an adjunct therapy.
Sure, it will be better than nothing, although I’m not sure of the best application time with something like a laser pointer. Good luck.
I have what I believe to be a low level localized recurring fungal infection that I can never quite get rid of. I have done every candida protocol under the sun and taken strong pharmaceutical antifungals as well as topical creams and I am fairly sure it’s not a gut issue as I experience no other fungal issues, rashes or any other skin conditions. More so now resistant candida from over treatment and low neutrophils from long term antibiotics.
I am considering doing red light therapy. My question is, is there such a thing as too much? As in would 10 minutes a night for a month be suitable or longer?
Secondly I found quite a few reference studies around methylene blue and light therapy as you mentioned but could not find a lot about safety when applying it topically, dilutions, dosages or anything like that. Small amounts seem to be safe orally but wondering how much of it penetrates the skin/how much is safe topically and given that it’s a dye, would it dye my skin if I used it night after night (I don’t want blue genitals haha),
I’ve only found a linear dose response relationship in the literature regarding how red light kills yeast. So the longer/more the better. I think up to an hour is a day is fine or until the skin starts to get warm, although just 20 minutes is probably enough.
I’m also not sure about the best dose of methylene blue for photodynamic therapy. I don’t think it will stain your skin for more than a few days max. I have noticed that using methylene blue and then applying red light afterwards on my skin gives quite an uncomfortable feeling, almost painful after a while. I would not recommend using it topically with red light therapy, because I think it may damage your own cells this way. Fungal cells already have an endogenous photosensitive pigment, so are suspecible to red light without needing the dye.
I think it is best to use methylene blue orally for metabolic reasons, and use red light separately.
Hey James. Did you have any luck with this? My situation sounds very similar and would love to know if anything helped..
I have an advanced fungal infection in my right ear that has spread to the right side of my head/mouth plus over prescribed antibiotics while living in France. I had success with castor oil both castor oil and the product Thorne 722 which is the direct active ingredient of castor oil. For the antibiotic damage saccaromyces boulardi specifically supported by other probiotics to rebuild my immune system. Peppermint essential oil to thin the biofilm. I did have a farinfared sauna which helped too but not without the castor oil. Back in the US now being treated by an ear doctor.
Hi
I have a yeast infection covering the whole right side of my right leg. It’s been going on for about three years. I did ha ve a whole body infection which I cleared up but as it started in the leg this is the most stubborn. I try everything but nothing works. the circle of the skin growing hard and building layers happens very quickly so I keep exfoliating it to keep it from turning into leather. I can see the little red yeast spots under the skin when I keep it exfoliated but it means sit is also in a constant state of inflammation so the vicious circle you speak about is ongoing. I have just bought a 300 watt infrared lamp and hope that by using this I may be able to kill it off eventually. Coconut oil and all that stuff has not gotten rid of it so I am at my wits end right now. I see how the skin is being damaged but feel helpless to really do anything to heal it. How long and how often would I need to use the lamp to see any improvement and a movement toward skin healing do you think in this situation?
Thanks
Maureen
Hi Maureen,
Wow, that sounds pretty bad. Sorry to hear about that.
I’m not sure if those infrared heat lamps are effective against yeast as such, at least I didn’t see any studies on that. I would guess that they probably have some effect though. Just stop using it before your skin gets warm. You mainly want visible red or near-infrared light, and not just a broad spectrum infrared bulb (which will contain all sorts of mid and far infrared heat wavelengths which are linked to photoaging). I’m not sure the 300w lamps will be useful in the same way or how best to use it for infections.
Have you tried castor oil?
Have you tried apple cider vinegar?
Just take 2 tablespoons with any kind of juice. (Besides orange juice). You don’t have to do 2 tablespoons but are used to take 1 teaspoon a day and now I take 2 tablespoons because it helps with my joints. The vinegar is known to cure yeast
Thanks so much for your response. I am completely confused now about the information above on how red light kills yeast with the diagrams pictures and graphs etc ? Could you recommend or point me in a direction of what device I should be looking for it I want to try this? There is so much conflicting information around the internet that it becomes nearly impossible to get a clear picture of how to use red light, and which wavelengths do what, that it begins to sound like smoke and mirrors :o)
Maureen
I am not able to make specific medical recommendations.
Studies indicate that a source of red or near-infrared light – 600-900nm wavelength – will work to help kill fungal cells and yeast in a lab.
Then you need that light to be in a higher intensity, upwards of 200mW/cm² will work best since there is a linear dose response (more light = more yeast killed).
I have a systemic fungal/candida infection. Chronic sinus infections, skin breakouts on arms, hands and face with itchy rashes, and toenail fungus, and am about 80 lbs+ overweight. I have been reading about light therapy, Near Infrared and Far Infrared mostly. From what I’ve read, Near Infrared is best to treat almost all health issues. But I’m getting confused with the “Red” light therapy and the “Infrared” light therapy discussed here. Please explain in layman’s terms the red and the infrared as compared to the near and far infrared light therapies. Then, if you would please, a recommendation for what is needed to deal with my health concerns/issues. Thank you.
Hi Heidi,
Red light therapy uses visible red light at 600-700nm wavelength. Infrared light therapy uses near infrared light at 700-900nm wavelength.
The far infrared you mention is not light, but is actually heat, at wavelengths of 15000nm to 1000000nm – vastly different to light. So far infrared is heat therapy, not light therapy. Far infrared doesn’t have the same biological mechanisms as red and near infrared.
My friend had almost the exact problems. A parasite cleanse along with red/infared light helped her… 🙏🏼
I have a pseudomonas aerignosa infection (antibiotic resistant) and wonder if red lights are harmful for this? It appears I need the blue light spectrum to kill it, but want to at least verify I’m not making it worse with red light? Thank you!
Hi Olivia,
Here is a study showing that near infrared inhibits the growth of Pseudomonas aeruginosa:
https://www.ncbi.nlm.nih.gov/pubmed/14651796
Wondering if using either the red or the infrared light will have any benefits of treating SIBO?
Hi Asif, I have not seen that studied much at all. I think it will help to at least some degree with the inflammation and symptoms, but I can’t say much more than that with certainty.
Take enteric coated peppermint capsules. Eat arugula salad.
Hi Joe,
You seem to be quite knowledgeable in all this so I trust your opinion.
I’m tickled pink to find this website.
I’ve recently purchased an irestorer system for hair since I’ve been losing so much of it and I really like the technology. Like Heidi, I have systematic Candida , trimethylaminuria and a cholestoma in my left ear that’s really bad. Would your 830 device be the best choice for me and do you ship to Canada.?
Thank you kindly for your time .
Nikki
Hi Nikki,
yes we ship to Canada, and I cannot make medical recommendations. All I will say is that the power, design and wavelength of the 830 Device give it the best penetration.
My Mother has oral thrush and it is resistant to medications. It seems the 830 would be the correct choice for her, but I am not sure if the mini 830 or the red 830 would be the best choice for her.
Also, how is this used for treating inside the mouth? Held near the outer skin surface or with the mouth open and exposed to the light?
Thank you J JONES
Hi Julie,
Unfortunately I cannot make medical recommendations like that.
Oil pulling with virgin coconut oil will help get rid of thrush.
Does this work for Vulvodynia as well?
It is not something I have seen studied specifically in regards to light therapy.
I have had jock itch for almost a year now, how many times a day and for how long should I do light therapy? My case of jock itch is mild.
I cannot make medical recommendations in regards to light therapy. Keeping the area dry is key (and I mean really dry).
I personally would use the red light in the morning until the skin is noticeably dry, then again after a shower/bath, even after going to the toilet, just to keep the skin permamently dry and reduce moisture throughout the day.
You should also considering using a low EMF fan to blow the area dry at the same time as applying the light.
After the treatment, applying a corn starch based baby powder to prevent any moisture build up as you go about your day is useful too.
How long you use it for
Could you please tell me which red light would be best for a fingernail infection, a 670 or 830? It looks like a fungus and has been cultured a few times but it never turns out to be a fungus. So maybe it’s a bacteria, I don’t know. Thank you!
Hi Lindsay, I think both of those wavelengths would be about equal in terms of killing off the yeast, and various other microorganisms. I think the main thing in addition to light therapy is keeping the area as dry as possible.
Hello,
Have you ever found any research on red light therapy curing tinea versicolor. It is a fungal infection and I stubborn one. Someone told me they cured their TV with blue light therapy, but I came across this website while researching and now I am curious if red light therapy can work for my TV.
Thank you.
I haven’t seen much on your specific condition, but there is one study:
https://www.worldwidejournals.com/indian-journal-of-applied-research-(IJAR)/file.php?val=September_2016_1492160593__159.pdf
They are not so specific about the wavelength, but they are using either a 670nm or near infrared source of light (based on the material they mention – Gallium Aluminum Arsenide). From the research I have seen on other yeast and bacteria, any wavelength in the 600-900 range should work.
It seems useful for your Versicolor condition according to this study, reducing itching and clearing up the scales in time.
The problem with blue light therapy, which does kill bacteria/yeast too, also harms your own cells, reducing immunity and increasing photoaging.
Hello, how would these products compare with the TDP lamp (can emit far infrared radiation that ranges from 2 to 50 micrometers)? Thanks in advance.
They are just completely different things. Like comparing radio waves to microwaves.
Far infrared is just a source of heat, heating water in your skin cells. Light therapy acts on your mitochondria, penetrating deeper than far infrared, and potentially increasing your own energy production and reducing inflammation.
HI: can this work for treat or cure fungus or yeast infection in my vulva area very near my vagina? Please let me know. Thanks
I have had toe nail fungus on my big toe for over 20 years and have everything to get rid of it. I even had my toe nail removed by a doctor and he used acid to burn the nerves to keep it from it from coming back, the toe nail grew back and I still have the fungus, it has spread to other toe nail on both feet. I just bought your Infared 830 device and am wondering how long and how often I need to use it on my toes?
I am not sure exactly.
The research I have seen shows a photodynamic effect in certain species of bacteria and fungi. If you are affected by a vulnerable species, than the more the better. Unfortunately I cannot give specific medical advice.
Thank you! I have been using the light for 10 minutes twice a day and am seeing a big improvement in only 2 weeks. I use it on both the top and bottom sides of my toes. I also used the light on my left hand that has arthritis and I was very surprised when I was totally pain free after only a few treatments, this was after suffering with the pain for the last 4 months with no relief no mater what I tried. Thank you for making an affordable, high quality light that works great!
cottagecharm11 what distance did you use for your treatments on your toe nails?
I have been having trouble for about a year and a half or two years.
It started with my two big toe nails curling and cutting into my skin. So I had them taken off by the Dr several times.
They would grow back and then do the same thing. It turned into obvious toe nail fungus.
* Which I have been treating with Tea Tree Oil and Vaseline. Slowly seems to be kind of clearing up.
Then I got jock itch, which i can not fully get over. Every so often I would get a new round of meds from the Dr and I seem to get 95 percent cured. But never 100 percent cured.
If I quit putting fungus cream on or spray the fungus comes roaring back.
Now it has started under my arms and a few weeks ago I got athletes foot so I freaked out and went to the Dermatologist who said * You are doing to much, just stop everything and come back next week.
The very next day, the Jock itch was red and spreading fast.
So I called the Dermatologist who said * You can put your meds back on and keep that appointment – for the next week.
I remember the Dermatologist kept saying / repeating over and over * Dry and Light , Dry and light.
So I found your Web Site about Red Light.
I have been using Red Light LED Waterproof Bulb for about a week.
I am seeing improvement. I have had on the inside upper thigh (Next to privates) a red line. That had never gone away , no matter what I do. That is almost 100 percent gone.
I had started showing signs of fungus on my neck. That is going down and lessening.
This morning I used a black light to see how I am doing. * I saw online that Black Light UV can show Fungus Infection.
Under my arms ( Arm Pits) is dark colored skin, Under my chin on neck is dark places.
Private parts are dark skin (Under black light) also upper thigh area.
What surprised me is my whole face (Under the Black Light) is dark skin.
Also the outside of my thighs (Which has always been a problem pimple area) The pimple/sores are black under the black light.
I do have a appointment again with the dermatologist in a couple weeks.
This can be depressing, I decided not to go to my Wifes family’s house this Christmas as I don’t want to give what I have to anyone . ( My Wife now seems to have athletes foot which seems to be clearing up with foot spray – she is visiting her family for Christmas)
Plus the fact that if you are visiting someone else’s house, shining Red Light on yourself will be difficult or a kooky thing to do . ( Having a Fungus outbreak would be even worse)
I am sitting around working on the computer with no pants on, shining Red Light all over myself every so often.
I am worried because I have read online that Fungus can be inside your lungs and go to all your organs .
(I have had a cough for a long time – I am thinking from smoking when I was young – I have quit smoking years ago) could be Fungus related.
With my Dermatologist who seems to have a * Less is more – Treatment Philosophy I am hopeful Red Light will put me over the top on getting over this.
I remember when I was young getting jock itch and getting over it with in a few days.
Now being over 50, it will not go away. Just seems to be getting worse. At least until I started using a LED Red Light Bulb ( Waterproof) it seems to be working slowly ( Slowly is better than being worse or staying the same) I thought I was holding at 95 percent cured when it was slowly getting worse and spreading.
I am hopeful now I am on the right track with Red Light. (Still using Spray / Cream when I sleep or need to go somewhere)
If I can get over it I may write a book and I am thinking about signing up as a affiliate. That is my hopeful thinking.
I hope you have changed your diet. Sugar feeds yeast and fungus. High carb foods create sugar too. Do a strict vegetable juice fast for a week or two you would be cured.
As the other commenter your diet must be cleaned up… only antifungal antibacterial anti-inflammatory diet with essentials oils that offer the same properties. Get yourself some MMS and start detoxing!
Hi, my husband has a real bad case of jock itch basically constantly during summer months. We have tried red light therapy and it seemed to help a bit.
We are also trying to get pregnant. Will the red light therapy have any effect on sperm production? Can it have negative side effects?
Thank you!
Something important is to get rid of the source of the Fungus contamination.
You can’t get over it if you are being Re-Infected , over and over etc.
In my case the source was a water bed.
I smelled mildew , so i took the water bed mattress out and there was water under it .
So, I threw out the waterbed mattress and used bleach to wash / clean the frame, checked with a UV light (Black light) to be sure it was all gone.
Laid out some cedar slats on the inside of the waterbed frame and ordered a Foam Mattress online and put that in.
Now, no more waterbed.
I also spray the bathtub out every time I use it with Bleach ( 1/2 Bleach and 1/2 water)
I use Red light twice a day , over toes, under arms, inside upper thigh and etc. I don’t shine very much if at all on privates as that can burn that area very quickly.
I also spray toes and inside upper thighs with Vinegar and water .
On two big toenails I put tea tree oil, then vicks vaper rub (Generic) then I seal that on the toenail with Vaseline. (Then spray toes with athletes foot spray) – if I am staying at home I also spray it under arms.
I also spray inside upper thighs with apple cider vinegar, I quit spraying privates with that as it burns the thin skin.
I spray there with that tough actin tanactin and use a creme inside upper thighs and I use a very tiny tiny bit of cream on base of penis
One thing I do is put socks on before under wear because the toenail fungus , if you dont have socks on and you put underwear on you will contaminate privates with the toenail fungus which will get on underwear from the toes (Which happened)
And I wash Underwear and socks separately, with bleach. (So as to not cross contaminate)
P.S.
That is what I am doing
i am getting better 🙂
Disclaimer: Check with your Dr, Pharmacist , etc etc etc and etc
Thanks for that Mr B. Great practical tips. I agree that finding the source, whether in your house or on your partner, etc., is very important.
One long term consideration, in addition to your advice, would also be re-establishing the normal microbiome. Just so you don’t have to spray yourself with vinegar every day forever.
In the vagina for example, the normal healthy state of the microbiome is for it to be dominated by lactobacilli bacteria, which prevent growth of candida and other yeast/bacteria. In chronic vaginal yeast infections, and bacterial vaginosis (BV), the dominant lactobacilli population is always deficient. They should make up roughly 50%+ of the total bacteria. You get infections there when their population drops to less than 50%.
After treating the infection, using something such as yoghurt to reintroduce species like lactobacillus acidophilus would help in long term resolution and prevent the infection returning.
P.S.
This morning I noticed something in the bathroom Sink drain , so I looked.
It looks like bathroom sink drain is full of green algae (Like you would see in a lake)
So the toothpaste and mouthwash that goes down the bathroom sink is feeding Fungus in the drain.
I poured the drain with bleach. Then I put something over the drain hole in the sink so the fumes from the bleach cant escape the drain.
So the drain trap in the sink is full of bleach.
I am doing that today to all my sink drains.
The fungus is in the house sewer pipes and the sink drains.
Bleach will get it out of there.
That is why I have a long term cough.
The Fungus is in the air from every sink drain in the house.
Bleach will cure that part of the Re-Infection.
Just think about it, modern humans spit toothpaste and mouth wash and also shaving cream all goes down the bathroom sink drain.
Fungus is eating that stuff and then the fungus in the sink drains keeps infecting people and they can’t get over it because it is coming from all the sink drains.
Fungus likes moist (Water) Dark (Inside our drains, pipes) and sugars (Sweet mouthwash, sweet toothpaste, and shaving cream.
Fungus does NOT like Bleach. Good thing here a Gallon of Bleach at the Dollar Store is $ 1.00
Bleach is poison and will encourage recurrence of fungus and mold. Use vinegar.
I already have heats lamps that operate at around 850 nm, so I get plenty of mitochondria-activating. (SaunaSpace). Should I just get the red light at 670nm? Your study is in 660nm why are your lights 670nm? Also, how many Joules do you get per minute and can these LEDs be put right on your skin?
thanks
A ‘heat lamp’ by definition does not operate at 850nm. If it did, it would not be hot. Thermal infrared starts at over 1000nm.
Heat lamps are also not useful for ‘mitochondria-activating’ or light therapy. They are not studied for photobiomodulation or proven at all. There might be a small overlap into some useful wavelengths, but the heating of the skin negates the benefits and encourages photoaging, eye damage, etc. If you measure the power density of the actual light therapy wavelengths from them, it is not sufficient. You can get sufficient power densities if you use them very close, but only at a range that would physically burn you in seconds. So they are definitely not suitable for deeper tissue, and not suitable for the skin either.
Any benefits you might notice from a heat lamp is likely from improved vasodilation due to being hot.
Red light at 670nm, from LEDs and lasers, is well studied for light therapy. There are hundreds of studies on both 660nm and 670nm.
The question about joules per minute does not make sense because the metric ‘joules per minute’ is not relevant to light therapy. Dosing is measured in Joules/centimeter squared and depends how far you use it from. The dose you receive (in J/cm2) is just a measure of the power density applied (in mW/cm2) and the time it is applied for.
HI: I have systemic candida throughout my whole body from taking too many antibiotics for lyme. What do you recommend using to get rid of candida and lyme. Thanks
I don’t know the solution for lyme disease. I have not seen any studies indicating that light therapy is useful for that.
Light therapy however, may potentially help with the mitochondrial damage that is a side effect of long term antibiotic use.
I have had patches of “warts” on the balls of my feet. I’ve had them for years and I’ve tried to treat them but they are very deep and therefore I apparently don’t get the root of them. They are becoming more and more painful. I’m wondering if the red light therapy would work for something like this.
Lugol’s iodine.
Orally or topically?
Hello,
Which of your product do you recommend best to treat Balanitis Xerotica (BXO)? I’m already in the middle of a treatment with my doctor and he uses some red light therapy to treat the area. 5 minutes and then 15 more with some cortisone cream. I was wondering if I can continue with the treatment with my personal lamp at home.
Thank you!
I do not make specific medical recommendations. If what you are doing is currently working, I would try to replicate that as closely as possible. For skin in general, red light is favoured over NIR.
Hello, would natural spectrum LED energy light (10,000 LUX) kill yeast infection? How is it compared with the red light?
Thank you!
Do you have any information or recommendations about the infrared/red light therapy and it’s effect on curing bacterial vaginosis? Have been suffering with it for three years and nervous to try because I’m afraid it may also grow the gardnerella bacteria or provide regeneration to the bad bacteria.
Also what is the difference between red and infrared light? I was confused and thought they do the same thing/have same effect.
Hi Joe. Could a laser pointer help with fungal infection in the ear? Do you have a product that can be used for this. Cheers
I don’t know. Maybe it could help a little. The important things are knowing the power density of the light, over what sort of area, and overall dose.
All of our products are within the power density range you might want to use on the ear. Personally I would consider the nir – 830nm range ideal for ear use. 100mW/cm2+
Hello. I have been suffering from vulvodynia for four yeasts after a bladder infection followed by a yeast infection from SEVERAL antibiotics. Since the initial yeast infection I now have burning and itching and redness and inflammation at the vestibule(opening of vagina) I ordered this red/infrared light. How should I use this and is this a good idea to use for this?
Hi Heidi,
Sorry to hear about these issues. I can only imagine how harmful this can be to quality of life.
While the origin of your problem seems to be from the infections and antibiotics etc., there must be a hormonal basis to support the continued growth of the candida. This type of thing usually flares up or appears about 1 week before the menstrual period. The cause would seemingly be the oestrogen hormone, which spikes around the same time, and supports the growth of candida by various mechanisms. Reducing oestrogen levels, in favour of progesterone, is the best long term aim.
There are studies with red/nir light on this type of thing. I think the most important consideration is to help your cells, without using a light so long as to dry out or irritate the area. I personally would favour a low to moderate dose in sensitive areas like the genitals, lips, eyes, etc.
hello, does red/infrared light help or hinder cystitis/uti. thankyou
How deep below the skin does the red and infrared light penetrate if you have the maximum light intensity for your most powerful product at the closest possible range, i.e. touching the skin?
If they can kill bacteria would there be a danger that you could kill the friendly probiotic bacteria in the gut?
It depends on the tissue type. A few inches at least. Even further for breast tissue, fat tissue, etc.
Red/inf light isn’t completely sterilising like ultraviolet – it only kills specific species of bacteria.
What type of bacteria does it not kill? Bifidus? Lactobacillus? These are the two main ones in your gut so if they survive and red light kills the ‘baddies’ that is amazing.
Side note – I’ve been suffering from prostatitis and allergies for years. I’ve tried RLT and I can say it’s moved the needle like nothing else, including Probiotics, Apple Cider Vinegar, Boric Acid suppositories, prostate massage, coconut oil suppository, KETO diet and even Diflucan! Red Light Therapy is an absolute miracle. I never thought I would cure this thing and now I have hope.
Joe, do you know if Red and IF light kills good bacteria like Bifidus and Lactobacillus?
Todd B
I performed a simple but effective test.
I took two probiotic pills. Webber Naturals 30billion pills I bought on Amazon for $13 for 30
I warmed up two equal sized glasses of milk.
I put one probiotic pill in each.
I shone a red light bulb which does 670nm and 830nm on one of the milk with probiotic (3 minutes)
I let them both sit in exactly the same environment
Two days later, the milk had firmed up equally in both glasses of milk
This tells me the red light did not destroy the probiotics in the milk in 3 min. I may perform this test with a longer light session on the milk.
Thought this was an interesting test anyone can perform at home easily to see if their light kills good bacteria as well as the bad guys.
Todd
I recommend also using a controlled glass of milk without any probiotic
Would it be useful for fungal acne?
Joe, do you know if Red and IF light kills good bacteria like Bifidus and Lactobacillus?
Todd B
Hi can red light cause a die off reaction when used on a yeast infection? I seem to be Herx’ing
Hi Stephen, I don’t know. I suppose so. I wouldn’t have expected such as strong response but it will depend on the degree of infection and exact species of yeast.
Hello,
i’m french, so excuse my english. Is red light good for wet AMD not dry AMD ? Which product for wet AMD and which protocol. Do you deliver to France? Thanks
There are studies for both dry and wet. Most of the studies use a 670nm light. https://redlightman.com/product/red-mini-670/
We do deliver to France.
Hi which device would be best for athletes foot? And how close should I put to skin and for how long?
https://redlightman.com/product/red-670-light-device/ – I would use this. As close as possible, 10 minutes, 2x per day.
Hi Joe,
What light would be the strongest/best for trying on a localised SIFO infection?
I know it seems hard to penetrate deeper than beneath the skin, but I’m willing to try it, in combination with my doctor’s treatment, based on the promising studies thus far.
Thanks.
This 830 Device pressed to the skin gives the deepest penetration into biological tissue:
https://redlightman.com/product/infrared-830-device/
Would you consider making vaginal light for internal use? There are a few on the market from China, but unsure of their effectiveness or quality. I feel there would be a market for this either for yeast infections or for vaginal healing following birth. Thank you, Michelle
We have considered it but couldn’t make a suitable one with current technologies. The problem with all internal or wearable devices is heat dissipation. If you make it low powered so that it doesn’t generate a lot of heat, then it is too weak for therapy. If you make it high powered enough to give suitably high light intensities, there is heat generation and you need heatsinks/fans to deal with that.
Hello. My naturopath is treating me for fungal issues that might be the cause of an ear issue I’m having (feeling of fullness), was wondering which of your products might help. Thanks
https://redlightman.com/product/infrared-830-device/
The wavelength – 830nm is well studied for deeper tissues of various types/sources (the studied areas include things like arthritis, brain trauma, injuries, knee/hip/back pain, oral issues, plus joint issues of various types). It penetrates well basically, goes deeper than red light.
The light intensity – this specific product uses a COB type LED chip, meaning there is a lot of light intensity coming out from a small area. It is infrared light, so you don’t see a bright light coming out, but readings when you measure it are off the charts high. This concentrated light is very dense and intense, meaning even better penetration and effects in deeper tissue. When you consider that only a small percentage of the light hitting the skin will penetrate down into the core of the body, it follows that you need to apply a very high dose – so this type of strong light with a concentrated light source helps with that.
The design – the large lens that comes to a point is ideal for the ears. You can just press the glass lens right into your ear and keep it there for a few minutes. It’s so easy to use because you can rest it on any flat surface and lie down or position yourself and your ear next to it.
Hello I just found this site after searching for infra-red light treatment. Read that 670nm would be ideal for “sunning the testicles” in order to boost testosterone production among other cool benefit. Would the Red mini 670 be up for the task?
https://redlightman.com/product/red-mini-670/
Yes it would be. Good choice. That’s the one we usually suggest.
What would be the best device to get for RECURRENT VAGINAL YEAST INFECTIONS? At what strength would you administer the device and for how long?
https://redlightman.com/product/red-670-light-device/
This 670 Device is most similar to lights used effectively in studies.
I would suggest sessions from quite close range, less than 5 inches, for around 5+ minutes. During flare-ups or active infection/inflammation/itching, I would do two sessions per day, after washing/shower. All you would need to do is lie down on a bed with the light also resting on the bed.
I know recurring vaginal yeast infections typically follow a predictable pattern around the menstrual cycle. During times when there is no itching, it would be advisable to at least do 4 sessions a week maintenance.
Do you ship to China?
Hi Mark,
Yes, we ship anywhere in the world, including China.
What would you recommend for a recurring balanitis? What light and how often ?
https://redlightman.com/product/red-mini-670/ – this would be the most suitable product.
Used 3-5 minutes, once per day from a distance of 15cm / 6 inches. Keeping foreskin in the normal position (if you have one), and not retracted.
Hi Joe. Why not retracted? Would it be harmful to expose the inflamed area directly to the red light?
One of the main functions of the mucus membranes of the human body (eyes, ears, inside the nose, inside the mouth, lip, vagina, glans penis/foreskin, the urethral opening and the anus) is to prevent bodily tissues from becoming dehydrated. Retracting the foreskin will cause the glans penis to dry out fairly quickly (which leads to irritation). Since red light will slightly increase the evaporation of water, using it directly on exposed mucus membranes like the glans penis and foreskin of an uncircumcised male will cause irritation. It’s not the red light that is directly causing harm, but the physical properties of how it accelerates moisture evaporation. Just keep the foreskin in the normal position to maintain the normal function and red light therapy will give the best benefits that way.
The 830 nm focused light (intense beam) has become my go-to tool for sore throats, ear infections, infected hang nails or stubborn facial outbreaks (zits) that won’t resolve; for any viral/bacterial infection, really, that I can shine this light on. I’ve been able to prevent development of full-blown infections and thus loss of time and need for antibiotics. I have toenail fungus, I applied this light daily for some months without any success.
For a fungal skin infection, how many times per day and how long each time would be good? I can’t find that information anywhere online. Any guidance would be appreciated.
Twice a day max. 5-10 minutes or more, depending on the strength of the light.
Hi, Joe just wanted to ask could I still use infrared light on my face if I have melasma? Thanks in advance
Yes you can. Using something like red or near infrared will keep inflammation low, which should reduce things like melasma in the long term.
Can infared light help with chronic uti? I have a antibiotic resistant infection
Possibly, although unknown. There isn’t comprehensive research on that. There is research on various other infections pointing to beneficial results.
Hey Joe! I am so lucky to find your website! I have been reading about red and IR therapy of skin rejuvenation and for general well being but not very very motivated about that. My daughter developed an adult acne after stopping the pill and she was treated for adult acne, but the location of the outbreaks on her upper back and neck , did not made sense to me. I suspected fungal folliculitis and the antifungals helped clear the outbreaks but shortly after stopping antifungal treatment started coming back. The dermatologist and the infectious disease specialist she visited have not even a clue. That is how bad the Western medicine has become.
I am not MD but being an European trained dentist I have very good understanding of the human body, not to mentioned being a motivated mom. I suspect the culprit is Malassezia Folliculits and need your help to choose the best light model you would recommend and how to use it: how many times, how much time and far from the light is the best to treat this fungus. It is on skin as a normal part of our skin microbiome, but when the sweat glands get infected causes an outbreak. Also is good to know how deep the light penetrates into the skin to be effective. And one more question: how the red and IR light affect the skin microbiome? What I mean is in reference with that famous Listerine commercial….Does the light kills the the “bad bacteria/fungus” , restores the normal flora or provides the immune system protects itself by improving the cells function. Sorry for the long post but I really need your advise because I am ready to place my order. Thank you!
Hi there!
Can you please tell me if red light works on bladder infections? If so, where would I point the light? Thank you very much.
I have a B.Light Restore Evo: This module uses a combination of 645 nm red light and 860 nm near-infrared light. I don’t know why I didn’t think about using this on a fungus between my fingers. I just started using it and the area is weeping clear fluid. Is this good? Will the fluid spread the fungus?